The Coronavirus Challenge
By Brian WoolfMay 23, 2020
The Coronavirus (or Covid-19) arrived on our doorstep early this year without an instruction manual. Looking around, we found two tools: The example of a societal lockdown in China (but without any medical details, infection or death rate data), and a computer-model of the Imperial College in London projecting over 2 million US deaths...
In our rush to respond, with only one society-management model on hand and without a better computer projection from our medical experts, we embraced both tools as our response's twin pillars.
Looking back, those two pillars may become an unfortunate part of our country's history because we have found that the computer's projection was egregiously wrong due to faulty modeling, and that a viable alternative to total lockdown was later developed and implemented by Sweden.
But such is past tense. More reliable computer models now project dramatically lower Covid-19 deaths and the Swedish model challenges the monolithic lockdown model from a combined medical and economic perspective.
We have also learned since embarking on this unsought journey that the people most vulnerable to the virus are the elderly (particularly those clustered in nursing homes) as they typically have the weakest immune systems to fight off a virus attack.
Indeed, all weak immune systems are, to some degree, vulnerable. As Wirepoints.org recently reported that Illinois's largest county, Cook County, recorded Covid-19 as the primary cause of death for 2,303 people. Of these, 92% had at least one underlying condition as a secondary cause (termed a "comorbidity"), eg, obesity, diabetes, hypertension, or heart disease.
Other studies indicate that young people are least susceptible to the virus and those in-between the young and the old are candidates to be virus carriers and test positive. How bad its effect on such carriers depends upon the strength of each person's immune system. We have learned that, overall, in any community some will have no symptoms, many people will have mild symptoms, some will have serious repercussions, and some will die. But at different rates in different states for different reasons.
Consider our Chinese-inspired total lockdown program. Its intent is avoiding inter-personal contact - maximum isolation for minimum contagion. Alas, that hasn't always worked out as pointed out by New York's Governor, Andrew Cuomo. In his daily press conference on May 5, he expressed shock that new Covid-19 hospitalizations of about 1,000 patients entering 100 New York state hospitals were from people who were staying home and not venturing much outside. A staggering two out of every three admissions (66%) were from those people who had largely been sheltering at home!!! A further one in five admissions (18%) were from nursing homes.
The Governor's pithy summation? Nearly 84% of our hospitalized cases were people who were not commuting to work through car services, personal cars, public transit or walking. A majority of these people were either retired or unemployed. And, overall, some 73% of the admissions were people over age 51. This shook our assumptions about the benefits of total lockdown.
To date, it seems that we have learned three lessons:
- Homes for the elderly should be ring fenced
- People with weak immunes systems should interact defensively
- All should practice social distancing, contact moderation, and cleanliness.
More lessons await learning, such as whether the 50 states should unlock from lockdown at their own chosen pace. So, to peer behind the politics and emotions of this question, I took a look at Covid-19 through the lens of numbers. What relevant Covid-19 hard numbers were common to all 50 states? I found three: population, area (in square miles), and Covid-19 deaths. To give them comparability, two metrics were added: the population density of each state (ie, how many people, on average, live in each square mile) and the CV-19 death rate (ie, CV deaths expressed as a percentage of its state's population.) All states data are listed in the two tables below (sorted from lowest to highest population density).
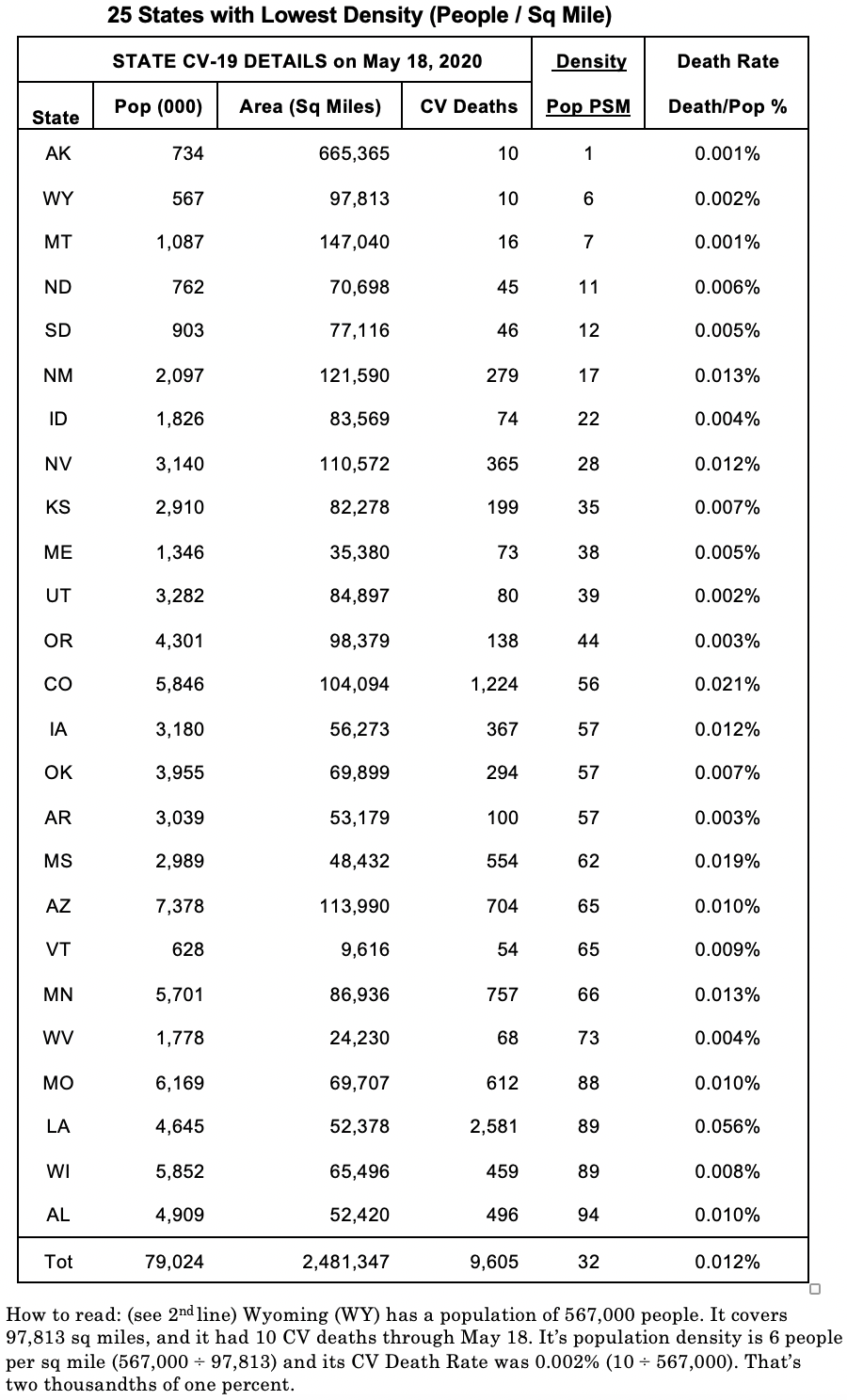
The key finding? Starting with Alaska (AK), our least dense state (1 person per sq mile), on to New Jersey (NJ), our most dense state (1,025 people per sq mile), the trend is that the more densely populated the state, the higher the CV death rate (ie, the higher the percentage of the population.) Covid-19 killed 0.001% (or one thousandth of 1%) of AK's population; in NJ, it killed 0.117% of its population, a rate more than 100 times worse. To provide perspective, consider the 90,649 CV deaths in the 50 states as at May 18. Now if all 50 states had AK's rate, the US death total would have been only 3,000 people. And if all had NJ's rate, it would have been 387,000, over 100 times higher. If you scan the right-hand column, you'll see how the death rate% increases as population density rises. No, it is not a perfect straight line-but it's a clear trend line.
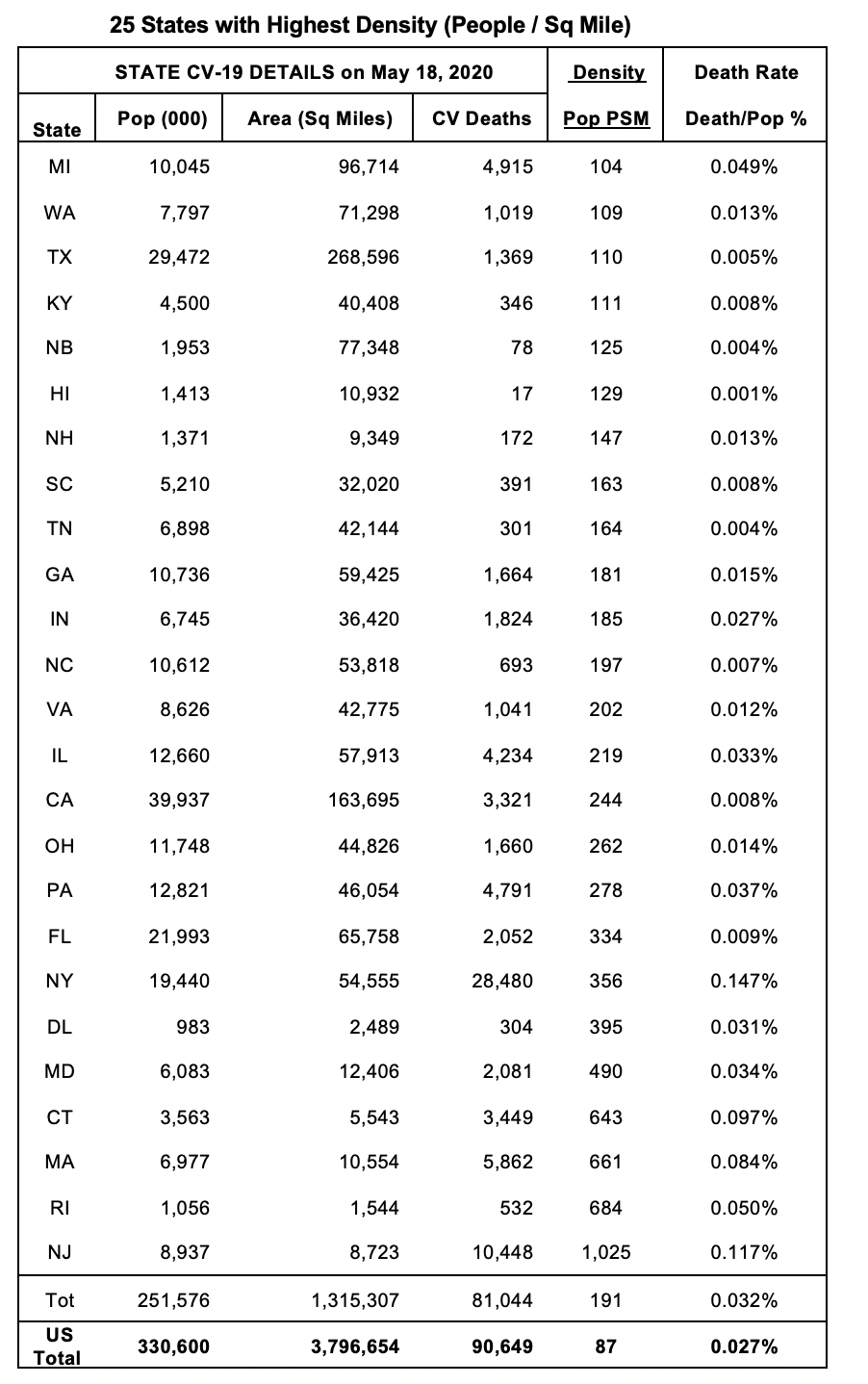
The numbers tell us that the denser a state's population, the higher its death rate.
Why? Why? Why? Any thoughts? I'll share mine in the next post.
About the author...
Besides a full business life in retailing, and later, loyalty marketing, the other part of Brian Woolf's life has been filled with diverse interests: particularly speaking (including Toastmasters), travel (including all seven continents), and reading (including history). And he has written seven books sharing what he has learned along the journey. Ask him, two favorite trips? Antarctica and the Nile. Ask him, two favorite books? The Lessons of History (Will & Ariel Durant) and Over the Edge of the World (Laurence Bergreen). He loves learning and sharing.

